2020 Annual Review
Message from the CEO
During 2020 we learnt many things. How resilient Victorians are, and how important our health is.
The focus for Cancer Council Victoria was to ensure our essential services could continue. Our 13 11 20 information and support line and our Quitline services remained running and were in high demand. Our cancer nurses dealt with large numbers of distressed calls from patients worried about COVID, about delays in treatments and from families navigating visitation access to loved ones in hospital.
Worryingly, there was a significant reduction in cancer notifications to our Victorian Cancer Registry. We know people were worried about attending medical appointments and there was a drop in screening. While we won’t know the full extent of this for some time, there is a concern this may result in late stage cancer diagnoses.
To help combat this we ran a ‘Don’t Delay’ campaign to encourage people to visit their health professionals and to screen for cancers like bowel and cervical.
I’m so very proud of the way our employees and supporters rallied last year. It was a difficult time for many, and we got through it together. We had to cancel many of our events and our fundraising was heavily impacted with people not able to support us in the same way.
You’ll see within this Annual Review what has been achieved over the past five years, and our vision for the next three in our new Strategic Plan for 2021-2023. This work can only be achieved with the support of fellow Victorians who want to see a cancer free future – thank you so much to everyone who has given their time, knowledge, passion, fundraising efforts and donations.
As you read through our Annual Review, I hope you feel proud of what we’ve achieved together.
Todd Harper
CEO
Cancer Council Victoria
Cancer in Victoria
A person is diagnosed with cancer every 15 minutes – that’s 98 a day.
11,000 Victorians die of cancer each year.
But survival is increasing… 69% of people now survive five years or more after a diagnosis.
In 2020 we spent:
$23.7 million on
cancer research
$16.6 million on
preventing cancer
$5.6 million on
supporting Victorians with cancer
Our Strategic Plan and achievements
Thanks to you, our supporters and stakeholders, since 2017 under our previous Strategic Plan thousands of Victorians have been supported through a cancer diagnosis, more cancers have been prevented, and more lives saved. See what you've achieved.
In 2020 we took the opportunity to review our Plan and refresh it to ensure we are able to achieve our goals and priorities with the changes the pandemic has created. View our new Strategic Plan 2021-2023.
What you helped us achieve in 2020
As part of our 2017-2021 Strategic Plan we have committed to four goals to achieve our mission of preventing cancer, empowering patients and saving lives.
Goal one: Implement powerful cancer prevention programs for major cancer risk factors: tobacco, UV, diet, obesity and alcohol
More than 6,424 lives were saved in 2020 thanks to improvements in treatments and the work of prevention programs including our Quit, SunSmart and healthy lifestyle campaigns.

UN honour for global cancer control work
A range of achievements using to law to prevent and control noncommunicable diseases (NCDs) have earned the McCabe Centre for Law & Cancer an award from the United Nations.
The 2020 UN Inter-Agency Task Force on the Prevention and Control of Noncommunicable Diseases (UNIATF) Awards recognise government agencies, UN country teams, and non-governmental organisations that make outstanding contributions to prevent and control NCDs at local, national, regional and international levels.
The McCabe Centre was one of 15 recipients in 2020, and the only recipient based in Australia.
“We are so grateful to be honoured for our efforts to address NCDs using law, and proud to share the honour with our fantastic partners and alumni,” Hayley Jones, Acting Director of the McCabe Centre said.
The McCabe Centre is the only centre of its kind in the world advancing law to fight cancer and other NCDs and promote equitable access to safe, effective and affordable care for people affected by them. Its work includes world-leading research and a capacity building program which since 2014 has trained more than 200 lawyers and policymakers from 70 countries on effective use of law to address cancer and other NCDs.
To date, alumni of the McCabe Centre training have gone onto support the passing of laws and/or regulations contributing to NCD prevention and control in 19 countries. Alumni in six countries have also successfully defended public health laws from legal challenges by the tobacco industry.
“Action to prevent and control NCDs has become more important than ever because of the COVID-19 pandemic, and we remain committed to working across sectors to respond to health issues and create sustainable change,” Jones said.
The McCabe Centre is a joint initiative of Cancer Council Victoria, the Union for International Cancer Control (UICC), and Cancer Council Australia, with staff based in Australia, the Philippines, Fiji and Kenya.

Investigating the harm of junk food marketing
A revolutionary new method is being developed to monitor how products that increase the risk of cancer are marketed to children thanks to donors to our $2.3 million Venture Grants program.
A team at Deakin University will create a world-first, automated approach for monitoring children’s exposure and engagement with advertising of products (alcohol, tobacco and junk food) known to increase the risk of cancer.
The World Health Organization recently identified a critical need for tools to monitor children’s exposure to and engagement with unhealthy advertising.
Lead researcher, Associate Professor Kathryn Backholer of Deakin University, said with the rise of digital and social media platforms, children are being exposed to high volumes of personalised and targeted marketing of alcohol, tobacco and junk food.
The tool will use cutting-edge AI technologies and eye tracking capabilities, which have been developed for use by Australian Defence and elite sports behavioural psychology.
Understanding how children engage with various forms of advertising and marketing strategies will support future policies to effectively protect children and the wider public health.
Protecting children from harmful exposure to unhealthy marketing is crucial to the prevention of cancer and a priority for Cancer Council Victoria.
A recent study by our behavioural scientists found that when unhealthy food and drink brands sponsor kids’ sport programs, parents are more likely to recognise, choose and view these brands in a positive light.
The study, published in Public Health Nutrition, tested over 1,300 Australian parents’ responses to simulated sponsorship of children’s sport by unhealthy food and drink brands. They compared it to two pro-health sponsorship options - healthier food branding and healthy eating campaign branding.
The study found that parents exposed to unhealthy food and drink sponsorship in kids’ sport were more than twice as likely to be aware of these brands than parents exposed to non-food brands. They were also almost twice as likely to choose unhealthy products when asked to choose a preferred food brand.
The research also found that they held more positive attitudes towards these unhealthy brands, viewing them as more aligned with the healthy, active image of kids’ sport.
Cancer Council Victoria’s Principal Research Fellow and lead researcher of the study, Associate Professor Helen Dixon said the research proved just how powerful sports sponsorship is in boosting the image and appeal of unhealthy food and drink sponsors’ brands.

Smoking falling but campaigns needed
Smoking among Victorian adults has almost halved since 2001, in part to decades of anti-smoking campaigns and advocacy for policy changes.
The Australian Institute of Health and Welfare’s (AIHW) 2019 National Drug Strategy Household Survey showed the daily adult smoking rate was 10.6% per cent, down from 12.3% in 2016 and 19.9% observed in 2001.
In 2007, just over 50% of the Victorian population had never smoked (53.5%) while in 2019, almost two-thirds of the population (63.8%) had never smoked.
The decline is driven by a large increase in the numbers of female never-smokers and 200,000 ex-smokers.
These successes are the result of Australia’s long-term commitment to comprehensive, evidence- based tobacco control measures, with the Cancer Council playing a leading role in the research, development and/or implementation of many of the measures.
The measures include bans on tobacco advertising, the introduction of plain packaging and enlarged graphic health warnings for tobacco products, smokefree public places, increases in taxes on tobacco products, innovation of Quitline counselling to support cessation, and public awareness campaigns that deter initiation of smoking and motivate people who smoke to attempt to quit.
Evidence shows us how often and how many advertisements are required to motivate people who smoke to seek advice and information to quit. There is a direct correlation between campaign levels on television and calls to the Quitline from people wanting to stop smoking.
The smoking prevalence could have been driven down further if public education campaigns had reached evidence-based levels over the past five to six years.
The number of Victorians who continue to smoke on an occasional basis is still a concern – while the prevalence of smoking within the population continues to fall, population growth means there is still a high number of Victorians who smoke.
There has also been an increase in the proportion of Victorian smokers who are using e-cigarettes, with pronounced usage among teenagers.
Goal two: Mobilise community participation in cancer screening and immunisation programs
Through our campaigns we want to increase participation in life-saving screening and immunisation programs.

COVID-19 slows down cancer notifications
There was a concerning drop in cancer reporting in the wake of COVID-19 restrictions.
Modelling by the Victorian Cancer Registry estimates that 2,530 cancer diagnoses were missed between 1 April 2020 and 15 October 2020, based on the registry receiving 5,446 (10%) fewer pathology notifications than expected over the period.
The impact of this number of potentially missed diagnoses is unknown, but any delay in cancer diagnosis for Victorians could mean their cancer is detected at a later stage, meaning potentially fewer treatment options and worse outcomes.
The most significant decrease in pathology notifications, and therefore likely missed diagnoses, occurred for head and neck, prostate and breast cancer and melanoma, in older Victorians, in men, and in people living in higher socio-economic areas.
Melanoma reporting to the Victorian Cancer Registry decreased by 31 per cent in the first period of restrictions in Victoria (30 March to 30 June 2020) compared to the pre-COVID period (1 Feb to 27 March 2020).
During 2020 there was increasing concern amongst health professionals that people with signs of cancer, and other health conditions, may not be contacting their doctors to discuss new symptoms.
The concerns prompted Cancer Council Victoria to develop its “Don’t Delay” campaign, urging people not to delay follow up appointments, to speak to their doctor if they had any health concerns and to continue cancer screening for breast, bowel and cervical cancer.
The campaign ran on TV, radio and online.
Cancer Council will continue to encourage Victorians to prioritise their health and work to increase participation in screening, one of the most effective ways to detect the early signs of cancer and increase survival.

More work to do in eliminating cervical cancer
Victoria is on track to become one of the first jurisdictions in the world to eliminate cervical cancer with a 48% drop in incidence since 1982, but we need to ensure elimination is achieved for all as some communities experience higher incidence and poorer health outcomes related to cervical cancer.
The statistics were revealed in the Victorian Cancer Registry’s latest report, the world’s most up-to-date look at cancer incidence, mortality and survival.
Cervical cancer is largely preventable thanks to both HPV vaccination and cervical screening, yet sadly 218 Victorian women were diagnosed with the disease in 2019.
While the National Cervical Screening Program, which began in 1991, has seen much success, a renewed screening program was introduced in December 2017. Data indicates that this renewed program is working, with a significant increase in pre-cancers detected with the current, more effective test.
The good news is also a result of the National HPV Vaccination Program. The report shows a significant decline in pre-cancer and invasive cervical cancer in young women, indicating the effectiveness of HPV vaccine.
But while we could be the first jurisdiction in Australia to eliminate cervical cancer, we need to focus on the inequities that exist in our society and prioritise communities that have lower screening and immunisation rates.
The introduction of self-collected HPV tests could increase screening rates for never-screened and under-screened women aged over 30. This method could be a significant tool to fast-track the equitable elimination of cervical cancer. Women should talk with their doctor or nurse cervical screening provider to see if they are eligible for self-collection. The test is easy to do and effective at detecting HPV.

'Cervical screening saved my life': Karina encourages others to screen
52-year-old Karina, a Leadership Coach based in Melbourne, is passionate about encouraging others to screen after her cervical cancer experience.
She had always participated regularly in cervical screening. Throughout her 30s, she had received a few abnormal Pap test results, which meant she was extra vigilant to prioritise screening.
Unfortunately, in the midst of organising her life to move back to Australia after a stint in the UK, she was diagnosed with a squamous cell cervical cancer tumour at the age of 39.
Link to https://www.cancervic.org.au/about/stories/karina-cervical-cancer.html

Gap not closed on cancer incidence, mortality
Both cancer incidence and mortality rates remain significantly higher for Aboriginal and/or Torres Strait Islander Victorians than in non-Aboriginal Victorians, according to the latest data from the Victorian Cancer Registry.
To reduce the incidence of cancer in the Victorian Aboriginal community, Cancer Council are working with the Victorian Aboriginal Community Controlled Health Organisation and other community organisations, with the community determining their own culturally appropriate strategies towards Closing the Gap.
Of the common cancers, for both men and women, rates are significantly higher for liver, lung, brain, bowel and head and neck.
Aboriginal women record higher rates of cervical cancer than non-Aboriginal women, along with pancreas, breast, uterus and vulva cancer.
Evidence shows that when the Aboriginal community determines and leads the implementation of strategies, then success can be achieved and sustained. Examples of this include the development and delivery of an Aboriginal comedy around bowel screening, Quit smoking animations and cancer screening resources.
Goal three: Empower patients by delivering dynamic, credible information and compassionate support
By 2033, nearly 48,000 Victorians will be diagnosed with cancer each year. Our services will grow and adapt to support them.

Nurses in high demand during COVID
Cancer patients and families experienced higher levels of distress and feelings of isolation during the COVID pandemic, with many turning to our cancer nurses for support.
Distressed callers to our 13 11 20 information and support line quadrupled, with many Victorians affected by cancer struggling with the impact of the pandemic on restrictions, delays in treatment and financial issues.
Our cancer nurses were on the frontline of our response to COVID with connections increasing from an average of 180 to 220 per week, with approximately half identifying COVID-19 as the primary reason for their contact.
Altogether, the nurses responded to 9,402 requests for information and support via calls and emails.
Thanks to donations from the Victorian community, our support services were there for everyone affected by cancer when they needed it most to provide emotional and practical support, as well as information about cancer treatments and how to navigate the health system during this challenging time.
Nurses reported a higher level of concern, with 80% of connections describing their distress as moderate (30%) to severe (50%), with levels peaking in April and June, coinciding with lockdown announcements.
Like Susan, who was pregnant with her fifth child when she was diagnosed with cancer. While she was undergoing chemotherapy, COVID-19 broke out.
Already taking care of four kids under six years old with another on the way, Susan said the additional challenges of COVID-19 had a significant impact on her cancer experience.
At the time Susan said: “It feels like cancer has to take a back seat; we have to deal with coronavirus. It’s lonely. All of a sudden it feels like all this support has just been pulled away from you.”
Finding it hard to find the support she needed during lockdown, Susan called 13 11 20 where she was linked to the services and support she needed.
Our cancer nurses were able to support patients like Susan, by helping them navigate the health system and restrictions, as well as linking them to essential services that could make a challenging time a little easier, and less lonely.
Nearly 500 people were supported by our pro bono financial and legal service in 2020, while our wig service was the only one operating. We adapted the service to be fully postal, with 291 people having a free wig mailed to them.

Vicki’s cancer diagnosis left her in financial distress
Vicki’s cancer diagnosis caught her completely by surprise and it quickly left her in financial trouble.
When a persistent cough hadn’t cleared, Vicki was sent for tests. Just a few days after her birthday, a PET scan confirmed the worst. She had aggressive stage 1 cancer in her lungs.
“It all happened so quickly. My head just spun. When you hear a diagnosis like that it’s true what they say. Your whole life flashes before your eyes in an instant.”
Within two weeks, Vicki was in hospital getting ready for life-saving surgery.
There’s no good time to get cancer, but the timing of Vicki’s diagnosis could barely have been worse. She’d only just moved into a new job in aged care.
Link to rest of story here: https://www.cancervic.org.au/about/stories/vickis-financial-distress.html
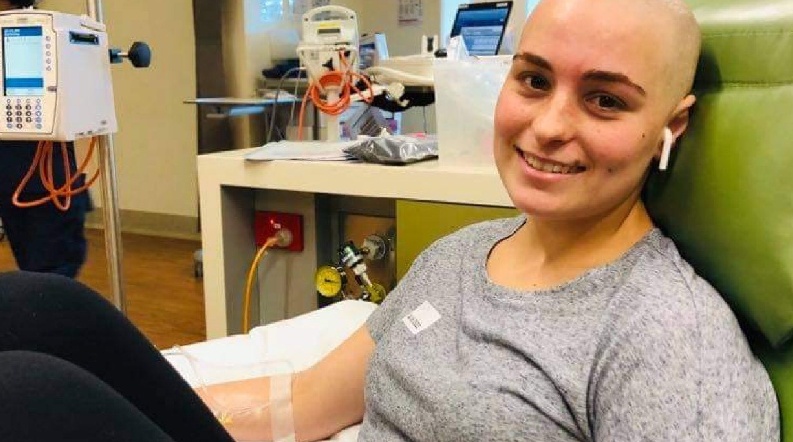
Somehow, Marnie kept smiling through COVID-19 and cancer
Marnie could never have predicted what 2020 had in store for her. At the beginning of the year, she was studying to become a nurse, taking classes with her dance company, and hanging out with friends.
“When I was diagnosed, it was a time in my life when I was just starting to find my feet and discover where I belonged in the world. Then it all came crashing down,” said Marnie.
In March, not only did she have to endure the shock of a Hodgkin’s Lymphoma diagnosis, she had to complete treatment through all the uncertainty and disruption of COVID-19.
“No one could come in [to the hospital] with me – I think mum came to my first treatment and from there I was on my own,” said Marnie.
“It’s pretty scary because you’re going into hospital not knowing what’s really going on and all by yourself, but I guess that’s how it had to be.”
Link to: https://www.cancervic.org.au/about/stories/marnies-story.html
Goal four: Maximise the impact of cancer research and cancer data
We are undertaking and investing in research to improve the way we prevent, detect and treat all cancers.

Generous gift gives hope for survival
A generous gift left by one of our donors has ensured immunotherapy will continue to improve treatments for patients for years to come.
Our $1.5 million Colebatch Clinical Research Fellowship was awarded to Associate Professor Shankar Siva, a radiation oncologist and scientist at Peter McCallum Cancer Centre.
The funding means cancer patients with advanced solid cancers could have access to a more precise, highly effective immunotherapy treatment within the next five years.
A/Prof Siva will use the five-year fellowship to investigate the use of a high precision technique called stereotactic ablative body radiotherapy (SABR) to ‘kickstart’ patients’ immune response, maximising the effects of immunotherapy.
A/Prof Siva’s research will include clinical trials investigating outcomes in patients with lung, kidney, prostate and breast cancers.
A/Prof Siva said the fellowship is critical for him to complete key studies and help pinpoint key factors in successful combination therapy.
“Immunotherapy is a major advance in cancer therapy, with the potential to improve outcomes in a range of different cancers. However, methods to improve the effectiveness of immunotherapy are urgently needed. This is where radiotherapy fits in.”
“I hope my research will significantly benefit cancer patients by providing them with access to effective, precision SABR + immunotherapy treatment, as well as identifying patients who are most likely to respond to this treatment.”
The fellowship was named in memory of Dr John Colebatch to mark his contribution to the Cancer Council and his work in the field of paediatrics. Dr Colebatch pioneered the use of chemotherapy in Australia in the 1950s to treat and, ultimately, cure childhood leukaemia.

We know more thanks to Health 2020
From alcohol to exercise, fatty acids to sugary drinks, we know more than ever about what affects our risk of cancer. Much of this is thanks to one extensive study – Health 2020.
Since 1990, Health 2020 – also known as the Melbourne Collaborative Cohort Study (MCCS) – has been investigating the roles of diet and lifestyle in causing cancer and other diseases using more than 41,000 Victorian study participants.
When the study began, diet and nutrition were considered potentially important factors affecting cancer risk, but there wasn’t much evidence to inform the prevention of the disease.
Thirty years and more than 900 scientific papers later, things have come a long way.
Some of the biggest breakthroughs of the Health 2020 study relate to body composition, diet and alcohol consumption.
“Health 2020 has been used to investigate associations between diet and a wide range of health outcomes,” Professor Roger Milne, Head of the Cancer Epidemiology Division at Cancer Council Victoria and Chief Investigator of the MCCS, said.
“The influence of dietary patterns has been investigated in relation to lung, bladder and breast cancer, type 2 diabetes, healthy ageing and more.”
By providing the evidence required to increase awareness of the health-related benefits and risks associated with dietary factors like alcohol, sugar, vegetables and fatty acids, Health 2020 is helping people make better choices to lower their risk of cancer.
In addition to these discoveries, Health 2020 made significant advances in understanding another factor: genetics.
“What we did not anticipate was the rapid growth in genomic technology and knowledge,” said Professor Graham Giles, the study’s Founding Investigator.
“Health 2020 blood samples became a highly valuable source of DNA to examine genetic risk factors for disease. This field of research has been our principal focus for the past 15 years.”
This led to the identification of hundreds of common genetic variants associated with the risk of more common cancers such as breast, bowel and prostate cancer, and to the discovery of many novel genetic variants linked to rarer cancers, like ovary and pancreas cancer.
Health 2020 is continuing to make such discoveries and have a global impact to this day.

Hope for ovarian cancer patients
New treatments for ovarian cancer are on the horizon thanks to generous donations which have helped fund Dr Holly Barker’s work at the Walter and Eliza Hall Institute.
Co-funded by the Ovarian Cancer Research Foundation (OCRF), the research will help improve survival rates for ovarian cancer which are currently at 47%.
The project, Identifying new treatment options for the rare and aggressive ovarian carcinosarcoma, is using a “unique toolbox” of pre-clinical models and screening technology which will allow new treatments to be tested.
While there is currently a range of treatments available for some ovarian cancers, fewer exist for ovarian carcinosarcoma (OCS). The rare incidence and lack of symptoms mean patients are often diagnosed at a late stage with treatments more suited for other types of ovarian cancers.
“Ovarian carcinosarcoma desperately needs better evidence-based treatment options. Through this project, we hope to challenge and refine the current treatment strategy for this rare, aggressive cancer. From this study, we can learn valuable lessons to benefit many rare cancer patients,” Dr Barker said.
OCRF CEO Lucinda Nolan said, “These types of partnerships allow the OCRF to bring funding into an area of ovarian cancer research that we might not otherwise be able to consider or fund. We hope this is another step-change in improving the treatment and outcomes for women with ovarian cancer.”
Research funding has been hit hard by the pandemic, so the generosity of the Victorian community ensures Cancer Council Victoria can continue to support projects, including for low survival cancers like ovarian.
Thank you to our supporters
Our volunteers, fundraisers and supporters enable us in everything we do. We thank them for their passion and commitment. View the list of our major supporters.

Will finds new way to fundraise in pandemic year
Will has been fundraising for those affected by cancer in honour of his loved ones since 2011, and he wasn't going to let a pandemic stop him in 2020.
He was just 12 years of age when his dad was diagnosed with cancer and his prognosis wasn't positive.
"It had already spread - they didn't know where it came from, but they assumed it started in the bowel. Then after an almost two-year battle he passed away shortly before my fourteenth birthday."
The now-28-year-old has also lost both of his grandpas, a friend from uni, and his family dog to cancer in the months and years that followed his dad's passing.
He decided to fundraise to honour them and "everyone else who has fought this horrible disease".
"At first, I set a very lofty target of $5,000 where I didn't know how long I would need to keep that page open to reach it, but I was going to come up with creative ways to raise those funds," Will said.
Over the nine years that followed, Will has raised an incredible $24,000 for Cancer Council through many fundraisers - ranging from easy ideas to the more ambitious.
The Warrnambool-based man also has walked the track at his local Relay For Life, volunteered at a Daffodil Day stall every year and even shaved his beard all for a good cause.
The cancelling of physical Relay For Life events and Daffodil Day sites in 2020 just made Will more determined than ever to fundraise.
He set up a video chat with his friends and family where they all took on a challenge to walk, run or paddle for 15 hours, checking in with eachother online along the way.
Will ended up walking 30km, with the whole team keeping the baton moving for 15 hours, from 5am to 8pm, doing 551km in total.
In a year with restrictions and challenges, Will's determination was incredible. And he's going to continue to raise money to help other families in the future.
"I saw how awful it was as a young boy losing my dad, and I don't think I'll ever forget the very end of life when they're in so much pain," explained Will.
"Finding out how to stop or slow one type of cancer, supporting one person that's fighting, or one family whose lost someone, anything like that is enough for me to keep fundraising."
Our board

Message from the chair
2020 tested all of us and while COVID impacted us in different ways, we know that cancer never stops.
I’d like to thank our staff, volunteers, supporters and partners, including the Federal and Victorian governments and VicHealth for getting us through a challenging year.
Cancer Council Victoria was able to be there for those who needed it most and we adapted our services for patients and families whether that be through assisting with virtual support groups or posting out wigs.
We took the opportunity in 2020 to refresh our Strategic Plan to set us up properly to deal with the future challenges post a difficult year.
Funding for the research sector has been hit hard, and Cancer Council Victoria has made a commitment to continue to invest in cancer research – something we can only undertake thanks to the generosity of the Victorian community.
COVID provides a useful perspective on the impact of cancer. In just over a year, 820 Victorians died from COVID. In 2019, 11,329—1300% more—died from cancer. We should not forget this. COVID was overcome with unprecedented public solidarity, public leadership and policy, widespread behavioural change, resource commitments, and in the end, harnessing research breakthroughs in genetic and immune science.
Overcoming cancer requires long-term vision and sustained investment into research. The behavioural and epidemiological research we do will help us to better understand and prevent cancer, while funding new treatments will benefit families for years to come.
I am buoyed by the strength and solidarity shown in Victoria in 2020 and I am hopeful of what we can achieve together in reducing the impact of cancer.
Professor Jeremy Millar
Chair of the Board
Board committees
The Board approves strategic directions, organisation structure, policies and implementation processes to ensure Cancer Council Victoria can achieve its mission.
Supporting them are the board committees:
-
Executive Sub-committee - Finance, Risk and Audit Committee
- Medical and Scientific Committee
- Standing Research Sub-committee
And our expert advisory committees:
-
Human Research Ethics Committee - Institutional Research Review Committee
- Venture Grants Scheme Committee
- Clinical Network
Our team

Epidemiologists pitch in to help COVID response
Epidemiologists were the rock stars of 2020, and a dozen of our Cancer Epidemiology Division staff were deployed to help with Victoria’s COVID-19 response.
As the pandemic began in Australia, health departments around the country recruited ‘surge’ workforces to support the huge amount of work required for disease prevention and surveillance. In Victoria, requests were made by the Department of Health and Human Services to universities and research institutes that had expertise in public health, and epidemiologists were in particular demand.
Our staff and students were involved in many aspects of the response, including data entry and cleaning, data analysis for politicians and the media and preparing the daily situation report for the Department of Premier and Cabinet and the Chief Health Officer.
They also assessed the epidemiological evidence to link cases and close contacts to known outbreaks, prepared reports on known outbreaks, and undertook rapid literature reviews to inform public health policy and strategy.
Deputy Head of Cancer Epidemiology, Associate Professor Brigid Lynch, said that Cancer Council Victoria staff and students were very pleased to be able to respond and help their community through this public health crisis. While the work was intense and there were tight deadlines, especially during the second wave, there was a strong sense of camaraderie amongst the team.
“We all learned a lot about health protection – how multidisciplinary teams are needed to respond to public health events, such as a pandemic. It was very interesting to see how field epidemiologists work on a day-to-day basis.
“For the most part I think we (as cancer epidemiologists) were mostly learning from the infectious disease epidemiologists and field epidemiologists. But as we got further into the pandemic, and we had time to really analyse the data to address specific questions, our causal inference knowledge and analytic skills were put to use.”
Our employees
Cancer Council Victoria promotes a diverse and inclusive workplace. We strive for excellence in how we undertake our work, ensure integrity in personal and professional behaviour and demonstrate compassion and respect for others.
Gender diversity
Female (292) - 80%
Male (73) - 20%
Cancer Council Victoria has introduced a third option of 'self-identify' for employees to select.
Gender balance of our executive team
Female (6) - 70%
Male (3) - 30%
Type of employment
Full time (206) - 60%
Part time (158) - 40%
Financials
Key financial results for 2020
Cancer Council Victoria recorded a net surplus for 2020 of $4.3 million. Total revenue reduced by $9.7 million largely driven by reduced charitable support from face to face events impacted by the pandemic.
An Accumulated Surplus of $47.4 million highlights a continuing healthy financial position.
At 31 December 2020, cash of $8.1 million and investments of $97.2 million were available to fund Cancer Council's operating activities. The reinvestment of income into diversified assets reduces liquidity risk for the organisation and maximises our ability to deliver significant and sustainable operational results in the future. An investment mandate designed to mitigate exposure to market losses is reviewed annually by management and Investment Committee members.
| Our finances (in millions) | 2019 | 2020 |
| Revenue from transactions | 77.8 | 68.2 |
| Expenses from transactions | (74.5) | (63.7) |
| Other comprehensive income | 5.3 | (0.2) |
| Net result from continuing operations | 8.6 | 4.3 |
| Total Assets | 120.3 | 122.3 |
| Net Assets | 86.6 | 90.9 |
| Accumulated Surplus | 41.5 | 47.4 |
| Reserves | 45.1 | 43.1 |
| Total Equity | 86.6 | 90.9 |
| Cash Flow ($ movement) | 6.5 | 0.1 |
Revenue
Where the money came from
Investment income in 2020 of $2.7 million has also contributed to the overall result.
Fundraising
2019 - $44.6 million
2020 - $29.7 million
2019 - $44.6 million
2020 - $29.7 million
External funding
2019 - $23.7 million
2020 - $22.6 million
2019 - $23.7 million
2020 - $22.6 million
Other
2019 - $9.5 million
2020 - $15.9 million
2019 - $9.5 million
2020 - $15.9 million
Fundraising income
Fundraising income was $27.9 million in 2020, which is $14.9 million lower than last year, largely driven by reduced charitable support from face to face events impacted by the pandemic.
Donations
2019 - $6.9 million
2020 - $6.6 million
2019 - $6.9 million
2020 - $6.6 million
Events
2019 - $11.6 million
2020 - $5.2 million
2019 - $11.6 million
2020 - $5.2 million
Bequests
2019 - $26.1 million
2020 - $17.9 million
2019 - $26.1 million
2020 - $17.9 million
Bequest income of $17.9 million was higher than the five-year rolling average of $15.0 million but down on the prior year result ($26.1 million in 2019).
Events income was $5.2 million.
Donation income was $6.8 million.
Bequest - $17.9 million
Events - $5.2 million
Donations - $6.8 million
External income
State funding has decreased by $1.2 million, this is driven by the delayed awarding of program funds in 2020.
State (inc VicHealth)
2019 - $16.9 million
2020 - $15.7 million
2019 - $16.9 million
2020 - $15.7 million
Commonwealth
2019 - $5.1 million
2020 - $3.6 million
2019 - $5.1 million
2020 - $3.6 million
Other
2019 - $1.7 million
2020 - $3.2 million
2019 - $1.7 million
2020 - $3.2 million
Expenditure
Where the money was spent
Total expenditure reduced by $10.7 million to $63.7 million in 2020. While overall Research, Prevention & Support program expenditure decreased by $10.2 million to $45.9 million to protect reserves, the organisation continued to invest in the strategic initiatives of bowel cancer screening, obesity prevention programs, support for cancer patients, as well as research grants for low survival cancers.
Cancer research
2019 - $29.1 million
2020 - $23.7 million
2019 - $29.1 million
2020 - $23.7 million
Cancer prevention
2019 - $20.1 million
2020 - $16.6 million
2019 - $20.1 million
2020 - $16.6 million
Cancer support
2019 - $6.9 million
2020 - $5.6 million
2019 - $6.9 million
2020 - $5.6 million
Fundraising
2019 - $13.4 million
2020 - $12.4 million
2019 - $13.4 million
2020 - $12.4 million
Other (including costs of retail)
2019 - $5.0 million
2020 - $5.04 million
2019 - $5.0 million
2020 - $5.04 million
Admin costs - 8%
Cost of Mission work - 73%
Cost of fundraising activities - 19%
Accumulated surplus and reserves
| Our funds (in millions) | 2019 | 2020 | |
| Accumulated surplus Accumulated Surplus increased by $5.9 million to $47.4 million. |
41.5 | 47.4 | |
| General reserve Capital profits derived from the sale of land and buildings. These profits are being allocated over time to build the capability of the organisation. |
11.6 | 9.8 | |
| Research fund Bequest funding where both capital and interest is restricted to research projects, and is allocated to projects over time. |
2.0 | 1.4 | |
| External grants Funding from competitively won grants and contracts where the project remains incomplete at year end. These funds are available to complete the designated projects only. |
12.7 | 14.8 | |
| Other restricted funds Donor funds received for specific projects not yet completed, and available only to complete those projects. |
7.9 | 7.5 | |
| Special funds Capital value of donations or bequests received with the condition that the funds be invested and only the incomes used for specific purposes. |
3.6 | 3.6 | |
| FVOCI (Fair Value Through Other Comprehensive Income) Reserve used to recognise increases and decreases in the fair value of investment assets through other comprehensive income. |
7.3 | 6.4 | |
| Total | 86.6 | 90.9 |
Tied vs untied income
Tied funds have restrictions on the program they may be applied against whereas there are no restrictions on untied funding.
The proportion of untied income has decreased this year from 66% to 64%.
Tied
2019 - $26.6 million
2020 - $24.7 million
2019 - $26.6 million
2020 - $24.7 million
Untied
2019 - $51.2 million
2020 - $43.5 million
2019 - $51.2 million
2020 - $43.5 million
Looking forward

The COVID-19 pandemic has had a material effect on the generation of fundraising income in 2020 and Cancer Council Victoria expects fundraising conditions to remain difficult into 2021. The strong financial position of the organisation combined with the JobKeeper program has allowed Cancer Council Victoria to develop a measured response to the changing operating conditions. The implementation of these COVID-19 response measures and the rollout of a new fundraising strategy will allow us to protect our core mission activity and continue the investment in new technology that will be essential in delivering our refreshed strategic plan.
A full set of Cancer Council Victoria financial audited financial statements can be downloaded from our website at www.cancervic.org.au/about/annual-report.
Fiona Green
Chair, Finance, Risk and Audit Committee

 Donate
Donate