Page last updated: January 2024
The information on this webpage was adapted from Understanding Skin Cancer - A guide for people with cancer, their families and friends (2024 edition). This webpage was last updated in January 2024.
Expert content reviewers:
This information was developed based on Australian clinical practice guidelines, and with the help of a range of health professionals and people affected by skin cancer:
- A/Prof Victoria Mar, Director, Victorian Melanoma Service, Alfred Hospital and Monash University, VIC
- Tracey Bilson, Consumer
- Raelene Buchan, Consumer
- Alison Button-Sloan, Consumer
- Dr Margaret Chua, Radiation Oncologist, and the Skin Radiation Oncology team, Peter MacCallum Cancer Centre, VIC
- Prof Anne Cust, Deputy Director, The Daffodil Centre, The University of Sydney and Cancer Council NSW Chair, National Skin Cancer Committee, Cancer Council, and faculty member, Melanoma Institute Australia
- A/Prof Paul Fishburn, Skin Cancer Doctor, Norwest Skin Cancer Centre, NSW and Faculty of Medicine, University of Queensland
- Danielle Goss, Melanoma Clinical Nurse Specialist, Amie St Clair Melanoma (part of Melanoma Institute Australia), Wagga Wagga, NSW
- Louise Pellerade, 13 11 20 Consultant, Cancer Council WA
- Dr Shireen Sidhu, Head of Dermatology, The Royal Adelaide Hospital, SA
- Dr Amelia Smit, Research Fellow – Melanoma and Skin Cancer, The Daffodil Centre, The University of Sydney and Cancer Council NSW
- Dr Tony Tonks, Plastic and Reconstructive Surgeon, Canberra Plastic Surgery, ACT
Many people feel shocked and upset when told they have skin cancer. We hope this information will help you, your family and friends understand how skin cancer is diagnosed and treated.
If you or your family have any questions or concerns, call Cancer Council 13 11 20. We can send you more information and connect you with support services in your area.
What is skin cancer?
Skin cancer is the uncontrolled growth of abnormal cells in the skin. The three main types of skin cancer are:
- basal cell carcinoma (BCC) – about two out of three skin cancers
- squamous cell carcinoma (SCC) – about one in three skin cancers
- melanoma – about one in 100 skin cancers.
BCC and SCC are also called non-melanoma skin cancer or keratinocyte cancer. They're far more common than melanoma and make up about 99% of skin cancers.
Melanoma starts in the melanocytes and is the most serious form of skin cancer because it is more likely to spread to other parts of the body, especially if not found and treated early.
Rare types of non-melanoma skin cancer include Merkel cell carcinoma and angiosarcoma. They're treated differently from BCC and SCC.
The skin
The skin is the largest organ of the body. It acts as a barrier to protect the body from injury, control body temperature and prevent loss of body fluids.
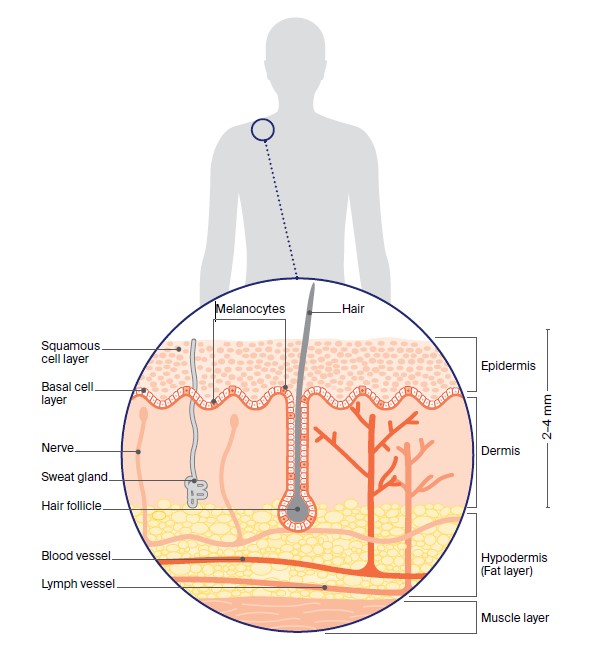
The two main layers of the skin are the epidermis and dermis. The epidermis is the top, outer layer of the skin. It contains three main types of cells:
- squamous cells – these flat cells are packed tightly together to make up the top layer of skin. They form the thickest layer of the epidermis.
- basal cells – these block-like cells make up the lower layer of the epidermis. The body makes new basal cells all the time. As they age, they move up into the epidermis and flatten out to form squamous cells.
- melanocytes – these cells sit between the basal cells and produce a dark pigment called melanin that gives skin its colour. When skin is exposed to ultraviolet (UV) radiation, melanocytes make melanin to protect the skin.
The dermis layer of the skin sits below the epidermis. It is made up of fibrous tissue and contains the roots of hairs (follicles), sweat glands, blood vessels, lymph vessels and nerves.
Both basal and squamous cells are keratinocyte cells, which is why non-melanoma skin cancers are sometimes called keratinocyte cancers.
Your guide to best cancer care
The guide to best cancer care for basal and squamous cell carcinoma can give you an overview of what to expect at every stage of your cancer care.
It's a short guide to what is recommended, from diagnosis to treatment and beyond.
Read the guide
What are the different types of skin cancer?
Basal cell carcinoma (BCC)
BCC usually grows slowly over months or years and only rarely spreads to other parts of the body. If left untreated, some BCCs can grow deeper into the skin, invade nerves and damage nearby tissue, making treatment more difficult.
Having one BCC increases the risk of getting another.
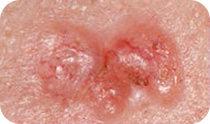
Signs of BCC
- Develops on areas that get more sun exposure, such as the head, face, neck, shoulders, lower arms and legs, but can occur anywhere on the body.
- May appear as a pink, pearl-like flat or raised lump or slightly scaly area that is shiny and pale or bright pink, or some may appear darker.
- The skin may break down (ulcerate), bleed and become inflamed. It may appear to heal and then become inflamed again.
Squamous cell carcinoma (SCC)
SCCs can grow quickly over several weeks or months. Invasive SCCs invade past the skin's top layer, and left untreated may spread to other parts of the body (metastatic SCC).
SCCs on the head, neck, lips and ears, and in people who are immunosuppressed, are more likely to spread.
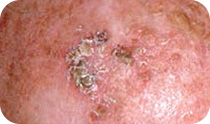
Signs of SCC
- Usually appears on parts of the body most often exposed to the sun, such as the head, neck, hands, forearms and lower legs, but can start anywhere.
- Often appears as a thick scaly lesion, a fast-growing pink lump, or a red, scaly or crusted spot
- May bleed and become inflamed, and is often tender to touch.
Other skin spots
Some spots that appear on the skin are not cancerous. If you are concerned about any mark or growth on your skin, see your general practitioner (GP) or a dermatologist to have it checked.
Sunspots (actinic or solar keratosis)
Sunspots occur more often in people over 40, but anyone can develop them. They usually appear on skin that’s frequently exposed to the sun, such as the head, neck, hands, forearms and legs.
Sunspots are a warning sign that the skin has had too much sun exposure. Very rarely sunspots may develop into SCC.
Signs of sunspots include:
- flat, scaly spot that feels rough
- often the colour of your skin or red.
Age spots (seborrhoeic keratosis)
These very common skin growths can occur anywhere except the palms and soles. They may look similar to a skin cancer or sunspot, but are harmless. They may be itchy and may bleed if scratched.
Signs of age spots include:
- raised area on the skin that feels rough
- may look and feel a bit like a wart
- light to very dark brown in colour.
Moles (naevus)
A mole (naevus) is a normal skin growth that develops when melanocytes grow in groups. Moles are very common. Some people have many moles on their body – this can run in families.
Overexposure to the sun, especially in childhood, can also increase the number of moles. People with large numbers of normal moles can have a higher risk of melanoma.
Signs of moles include:
- brown, black or the same colour as your skin
- usually round or oval.
Irregular mole(dysplastic naevus)
People with many irregular moles (dysplastic naevi) may have a greater risk of developing melanoma.
Signs of dysplastic naevi include:
- a larger mole with an irregular shape and uneven colour.
“I have lots of age spots and moles. I find it hard, but I try to keep track of what they look like, and any changes. But I make sure to get a skin check by a doctor every year too. Last check they found an SCC, but luckily it was treated early.” GWEN
Causes
Over 95% of skin cancers are caused by exposure to UV radiation. When unprotected skin is exposed to UV radiation, how the cells look and behave can change.
Across Australia, the UV levels can do damage to unprotected skin most of the year, not just in warmer months. UV radiation can’t be seen or felt, and can cause sunburn; premature skin ageing; and damage to skin cells, which can lead to skin cancer.
You can’t always see sun damage that’s happened to the skin – it can happen long before you get sunburnt or develop a tan. The damage also adds up over time and can’t be reversed.
You can check the UV levels in your local area on the SunSmart app.
How common is skin cancer?
Australia has one of the highest rates of skin cancer in the world. About two in three Australians will be diagnosed with some form of skin cancer before the age of 70 (Australian Institute of Health and Welfare).
Non-melanoma skin cancer is the most common cancer diagnosed in Australia. Over one million treatments are given each year in Australia for non-melanoma skin cancers.
BCC can develop in young people, but it is more common in people over 40. SCC occurs mostly in people over 50.
Risk factors
Anyone can develop skin cancer but it’s more common as you age. Many factors can increase your risk, including having:
- pale or freckled skin, especially if it burns easily and doesn’t tan
- red or fair hair and light-coloured eyes (blue or green)
- unprotected exposure to UV radiation, particularly a pattern of short, intense periods of sun exposure and sunburn, such as on weekends and holidays
- actively tanned, sunbaked or used solariums
- worked outdoors or spent a lot of time outside (e.g. gardening or golfing)
- been exposed to arsenic
- a weakened immune system – this may be from having leukaemia or lymphoma or using immunosuppressive medicines (e.g. for rheumatoid arthritis, another autoimmune disease or for an organ transplant)
- lots of moles, or moles with an irregular shape and uneven colour
- a previous skin cancer or a family history of skin cancer
- certain skin conditions such as sunspots, because they show that you have had a lot of skin damage from exposure to the sun
- smoked cigarettes, as smoking has been linked to a possible increase in skin cancer risk.
People with brown, black, olive or very dark skin have more protection against UV radiation because their skin produces more melanin than fair skin does. However, they can still develop skin cancer.
Learn how to reduce your risk