What is ACC?
Adenoid cystic carcinoma (ACC) is a rare type of cancer that forms in glandular tissues most commonly in the head and neck, but it can also begin in other areas. ACC often starts in the salivary glands in the neck, mouth or throat, which make saliva. Saliva keeps the mouth moist, helps you swallow food and protects the mouth against infections.
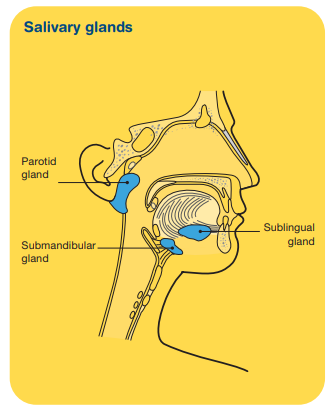
There are three pairs of major salivary glands and hundreds of minor salivary glands throughout the lining of the mouth and throat. The major salivary glands include:
- parotid glands – in front of the ears
- sublingual glands – under the tongue
- submandibular glands – under the jawbone.
How common is ACC?
ACC is rare and may account for up to a quarter of salivary gland malignancies. Around 330 Australians are diagnosed with a salivary gland cancer each year (1.2 cases per 100,000 people). Estimates of 0.3 to 0.5 cases per 100,000 people each year have been reported for ACC in other countries.
While ACC can develop at any age, it is more common in people 40 to 60 years old. Slightly more females are diagnosed than males.
Learn more about rare cancer
Symptoms
The cause of ACC is not known. It might develop from genetic changes that happen during a person’s lifetime, rather than inheriting a faulty gene. ACC is not considered to be hereditary.
ACC generally develops slowly, sometimes over several years, and may not cause symptoms. Most often it is diagnosed as a single tumour but may have spread to nearby lymph nodes by the time it is diagnosed in a small number of cases.
Rarely, ACC can spread along nerves or metastasise to other parts of the body (usually the lungs, liver or bone) and cause problems. It can also be unpredictable, growing slowly for a period of time and then suddenly growing quickly. ACC may behave differently in different people.
If you do have symptoms, it will depend on where in the body the tumour is located and its size. Symptoms may include:
- Salivary gland (produces saliva) – painless lump in the mouth, face or neck, numbness in the face, weakness in facial muscles and problems swallowing or opening mouth.
- Lacrimal gland (produces tears) – bulging eye and changes in vision.
- Larynx (voice box) and trachea (windpipe) – hoarseness, changes in speech and difficulty breathing.
- Skin – pain, increased sensitivity, pus and/or blood discharge.
- Breast – slow growing lump that may be tender or cause pain.
Diagnosis
If your doctor thinks that you may have ACC, they will take your medical history, perform a physical examination (including feeling for any lumps) and carry out certain tests depending on the location of the suspected tumour. If the results suggest that you may have ACC, your doctor will refer you to a specialist for more tests.
Further tests
Further tests a specialist may carry out include:
- CT (computerised tomography) and/or MRI (magnetic resonance imaging) scans – special painless machines are used to scan and create pictures of the inside of your body. You may have an injection of dye into one of your veins, which makes the pictures clearer.
- PET (positron emission tomography) scan – you will be injected with a small amount of radioactive glucose (sugar) solution to help cancer cells show up brighter on the scan.
- Ultrasound scan – soundwaves are used to create pictures of the inside of your body.
- Biopsy – removal of some tissue from the affected area for examination under a microscope.
Finding a specialist
The Australian and New Zealand Head and Neck Cancer Society can be contacted for a directory of specialist teams in ACC care and treatment. Rare Cancers Australia have a directory of health professionals and cancer services across Australia. The Adenoid Cystic Carcinoma Research Foundation (ACCRF) have a global list of specialists in ACC treatment, including those in Australia.
Treatment
You will be cared for by a multi-disciplinary team of health professionals during your treatment, which may include a surgeon, radiation oncologist, speech pathologist and dietitian, among others. Discussion with your doctor will help you decide on the best treatment for your cancer depending on:
- where it is in your body
- whether or not the cancer has spread (stage of disease)
- your age, fitness and general health
- your preferences.
The main treatments include surgery, radiation therapy and chemotherapy. These can be given alone or in combination. Surgical removal of the cancer with follow-up radiation is the standard treatment for ACC where there is a primary tumour.
Complementary therapies are designed to be used alongside conventional medical treatments (such as surgery) and can increase your sense of control, decrease stress and anxiety, and improve your mood.
Surgery
Surgery is usually the most effective treatment for ACC if the cancer can be safely removed. Surgery usually involves removing the cancer and some healthy tissue around the cancer. This is called a wide local excision. The healthy tissue is removed to help reduce the risk of the cancer coming back in that area.
The extent of the operation depends on where the cancer is and how far it has spread. The surgeon will examine nearby nerves and lymph nodes and may remove them if they are involved. It can be a difficult decision to remove nerves, especially major nerves or those that control the face.
Radiation therapy
Radiation therapy uses high energy rays to destroy cancer cells. It may be used effectively for ACC after surgery, to destroy any remaining cancer cells and stop the cancer coming back. It might also be used alone if surgery is not possible, for example:
- if the cancer is in a place in the body that is too hard to reach using surgery
- if the cancer has spread to other parts of the body (e.g. palliative radiation for the management of pain).
A course of radiation therapy needs to be carefully planned. It does not hurt and is usually given in small doses over a period of time to minimise side effects.
Chemotherapy
Chemotherapy is not commonly used for ACC. It may be considered when the cancer is advanced as part of palliative treatment or as part of a clinical trial. Your medical oncologist will discuss options with you.
Chemotherapy is given through a drip into a vein (intravenously) or as a tablet that is swallowed. It is given in treatment cycles which may be daily, weekly or monthly. The length of the cycle and number of cycles depends on the chemotherapy drugs being given.
Side effects
All treatments can have side effects. The type of side effects that you may have will depend on the type of treatment and where in your body the cancer is. Some people have very few side effects while others can have more. A speech pathologist and/or dietician may be able to help.
After surgery or radiation therapy to the head and neck area, you may need to adjust to significant changes. Some long-term side effects of treatment to this area include:
Common side effects relating to specific treatment types include:
- Surgery – bleeding, damage to nearby tissue and organs (including nerves), drug reactions, pain, infection after surgery, blood clots, weak muscles, lymphoedema.
- Radiation therapy – fatigue, loss of appetite, nausea, hair loss, dry mouth, skin problems, lymphoedema.
- Chemotherapy – fatigue, loss of appetite, nausea, bowel issues such as constipation or diarrhoea, mouth sores, skin and nail problems, increased chance of infections, loss of fertility, early menopause.
Question checklist
Asking your doctor questions will help you make an informed choice about your treatment and care. You may want to include some of the questions below in your own list:
- How far has the cancer spread? What stage of cancer do I have?
- Have you treated this type of cancer before? If so, how many times? Is there another doctor who has more experience treating this type of cancer?
- What treatment do you recommend and why?
- What are the possible risks and side effects of my treatment? How will these be managed?
- How long will treatment take? Will I have to stay in hospital?
- Is this treatment covered by Medicare/private insurance? Will there be extra expenses?
- Will I have a lot of pain with the treatment? What will be done about this?
- Will my face or neck have significant scarring or will I look different? What can be done to minimise this?
- What kind of rehabilitation will be available to me afterwards?
- Are there any complementary therapies that might help me?
- What are the possible benefits and risks to joining a clinical trial? What is being tested and why? How many people will be involved in this trial?
Life after treatment
Once your treatment has finished, you will have regular check-ups to confirm that the cancer hasn’t come back. Ongoing surveillance for ACC involves a schedule of ongoing blood tests and scans. Maintaining a healthy body weight, eating well and being active are all important.
For some people ACC does come back after treatment, which is known as a recurrence. It may also spread to other parts of the body after a couple of years. If the cancer does come back, treatment will depend on where the cancer has returned to in your body and may include a mix of surgery, radiation therapy and chemotherapy.
In some cases of advanced cancer, treatment will focus on managing symptoms, such as pain, and improving your quality of life without trying to cure the disease. This is called palliative treatment.
Learn more
Understanding Adenoid Cystic Carcinoma
Download our Understanding Adenoid Cystic Carcinoma fact sheet to learn more
Download now
Expert content reviewers:
A/Prof Dion Forstner, Radiation Oncologist, St Vincent’s Hospital, Sydney, NSW; Nick Kelly, Consumer; Caitriona Nienaber, 13 11 20 Consultant, Cancer Council WA.
Page last updated:
The information on this webpage was adapted from Understanding Adenoid Cystic Carcinoma (ACC) - A guide for people affected by cancer (2021 edition). This webpage was last updated in September 2021.