Kidney cancer
Kidney cancer is cancer that starts in the cells of the kidney. About 9 out of 10 kidney cancers are renal cell carcinoma (RCC), sometimes called renal cell adenocarcinoma. RCCs start in the cells lining tiny tubes in the kidney’s nephrons.
In the early stages of RCC, the tumour is in the kidney only. Usually one kidney is affected, but in rare cases there is a tumour in both kidneys. As the cancer grows, it can spread to the surrounding fatty tissue, veins, adrenal glands, lymph nodes, ureters or the liver. It may also spread to other parts of the body, such as the lungs or bones.
About the kidneys
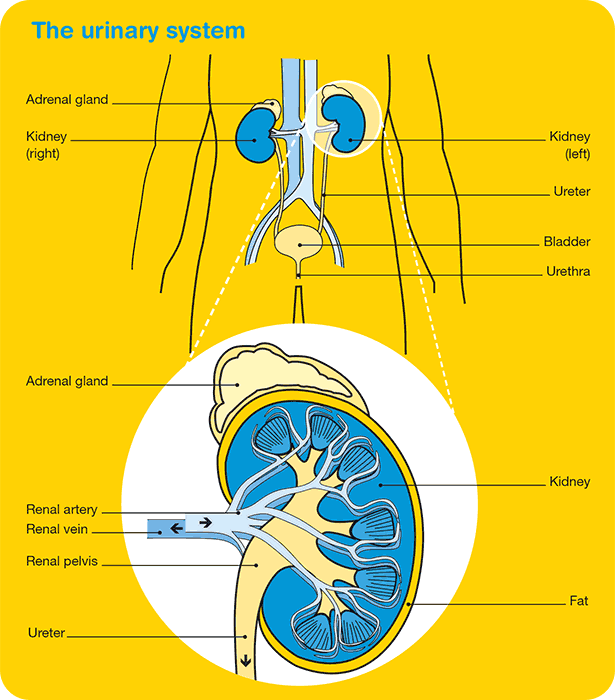
The kidneys are two bean-shaped organs, each about the size of a fist. They are deep inside your abdomen, positioned near the middle of your back, on either side of the spine. The kidneys are part of the body’s urinary system.
What the kidneys do
The main role of the kidneys is to filter and clean the blood. Blood flows into each kidney through the renal artery and is filtered through tiny networks of tubes called nephrons. The clean blood then goes back into the rest of the body through the renal vein.
When the kidneys filter the blood, they remove excess water and waste products and turn these into urine (wee or pee). Urine travels from each kidney into a funnel called the renal pelvis, then through a long, thin tube called the ureter, and into the bladder. Urine is stored in the bladder until you need to urinate, when it leaves the body through a tube called the urethra.
In females, the urethra is a short tube in front of the vagina. In males, the tube is longer and passes through the prostate and penis.
- Hormone production – the kidneys also help your body control how much blood it needs. They do this by making hormones that regulate blood pressure and trigger the production of red blood cells.
- Adrenal glands – an adrenal gland sits above each kidney. The adrenal glands produce a number of hormones. Although these glands are not part of the urinary system, kidney cancer can sometimes spread to them.
How common is kidney cancer?
More than 3600 people are diagnosed with kidney cancer in Australia each year. It makes up about 2.5% of all cancers. It is twice as common in men as in women, and is the sixth most diagnosed cancer in Australian men.
The risk of kidney cancer increases with age, and most cases occur in people over 50.
Learn more about kidney cancer statistics and trends
Types of kidney cancer
There are several types of RCC, based on how the cells look under a microscope:
- Clear cell (about 75% of RCC cases) – cancer cells look empty or clear
- Papillary (about 10-15% of RCC cases) – cancer cells are arranged in finger-like fronds
- Chromophobe (about 5% of RCC cases) – cancer cells are large and pale
- Other types of RCC (about 5-10% of RCC cases) – including renal medullary carcinoma, collecting duct carcinoma, MiT family translocation RCC, sarcomatoid RCC and other very rare types.
RCC is the most common type of kidney cancer, but there are other less common types:
- Urothelial carcinoma (or transitional cell carcinoma) – this can begin in the ureter or in the renal pelvis, where the kidney and ureter meet. Urothelial carcinoma of the kidney or ureter behaves and is treated like bladder cancer (another type of urothelial cancer), rather than like RCC.
- Wilms tumour (or nephroblastoma) – this type of kidney cancer is most common in younger children, but it is still rare.
- Secondary cancer – very rarely, cancer can spread from the original (primary) cancer to the kidney. This is known as secondary cancer (metastasis). This secondary cancer is not kidney cancer and it behaves more like the original cancer.
Symptoms
Most people with kidney cancer have no symptoms and many are diagnosed with the disease when they see a doctor for an unrelated reason. Symptoms can include:
- blood in the urine (haematuria) or change in urine colour – can be dark, rusty or brown
- pain in the lower back or side not caused by injury
- a lump in the abdomen
- constant tiredness
- unexplained weight loss
- fever (not caused by a cold or flu).
Cancer can affect the amount of hormones produced by the kidneys, and this may lead to a low red blood cell count (anaemia), a high red blood cell count (polycythaemia) or high levels of calcium in the blood (hypercalcaemia). Sometimes these problems can cause symptoms such as fatigue, dizziness, headaches, constipation, abdominal pain and depression.
The symptoms listed above can also occur with other illnesses, so they don’t necessarily mean you have kidney cancer – only testing can confirm a diagnosis. If you are concerned, talk to your doctor.
Risk factors
The exact causes of kidney cancer are not known. However, these factors may increase the risk:
- smoking – people who smoke have almost twice the risk of developing kidney cancer as non-smokers. About 1 in 3 cases of all kidney cancers are thought to be smoking-related. The longer and more frequent a person smokes, the greater the risk.
- obesity – too much body fat may cause changes to some hormones that can lead to kidney cancer.
- high blood pressure – whatever the cause, high blood pressure increases the risk.
- kidney failure – people with end-stage kidney disease have a higher risk.
- family history – people with a parent, brother or sister (first-degree relative) with kidney cancer are at increased risk.
- inherited conditions – about 2–3% of kidney cancers develop in people who have particular inherited syndromes, including von Hippel–Lindau disease, hereditary papillary RCC, Birt–Hogg–Dubé syndrome and Lynch syndrome.
- exposure to toxic substances at work – the risk may be higher after regular exposure to chemicals, such as some metal degreasers, arsenic or cadmium, which are used in mining, farming, welding and painting.
Having these risk factors does not mean you will develop kidney cancer. Some people develop kidney cancer without having any known risk factors. If you are concerned, talk to your doctor.
Health professionals
Your GP will arrange the first tests to assess your symptoms. If these tests do not rule out cancer, you will usually be referred to a specialist such as a urologist, who will arrange further tests. If kidney cancer is diagnosed, the specialist will consider treatment options.
During and after treatment, you will see a range of health professionals who specialise in different aspects of your care, which may include a nephrologist, radiologist, dietician and physiotherapist, among others.
Understanding Kidney Cancer
Download our Understanding Kidney Cancer booklet to learn more
Download now
Expert content reviewers:
A/Prof Daniel Moon, Urologic Surgeon, Australian Urology Associates, and Honorary Clinical Associate Professor, The University of Melbourne, VIC; Polly Baldwin, 13 11 20 Consultant, Cancer Council SA; Ian Basey, Consumer; Gregory Bock, Urology Cancer Nurse Coordinator, WA Cancer and Palliative Care Network, North Metropolitan Health Service, WA; Tina Forshaw, Advanced Practice Nurse Urology, Canberra Health Services, ACT; Dr Suki Gill, Radiation Oncologist, Sir Charles Gairdner Hospital, WA; Karen Walsh, Nurse Practitioner, Urology Services, St Vincents Private Hospital Northside, QLD; Dr Alison Zhang, Medical Oncologist, Chris O’Brien Lifehouse and Macquarie University Hospital, NSW.
Page last updated:
The information on this webpage was adapted from Understanding Kidney Cancer - A guide for people with cancer, their families and friends (2020 edition). This webpage was last updated in September 2021.